
Logout
If you want to log out click in LogOut


Maintaining immune homeostasis is achieved through the control of the magnitude of immune responses, itself regulated by the balance between co-stimulatory and inhibitory signals.
These signals are initiated by immune checkpoint molecules, whose activation regulates antigen-specific T cell responses against malignant cells or pathogens by affecting many signalling pathways(1).
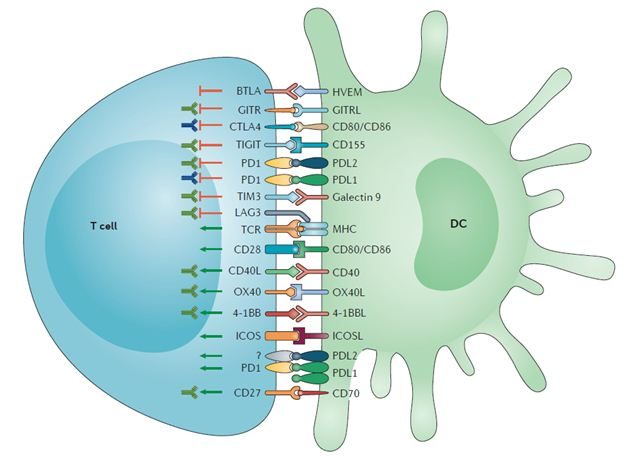
Among these factors, programmed cell death protein 1 (PD1) and cytotoxic T lymphocyte antigen 4 (CTLA4), receptors that negatively regulate T-cell activation(2-3) and tricked by cancer cells, were rapidly proposed as key biomarkers to cancer immunotherapy in order to boost the immune response against tumor cells.
Clinical success of immune checkpoint blockade in cancer opens up to new promising therapies in many other diseases as acute infections that leads to the upregulation of immune checkpoints(4), like malaria, chronic persistent viral infections, including HIV and hepatitis B virus...
However, as only a subset of patients respond to immunotherapies in cancer(5), monitor the gene expression of such biomarkers could predict responses to these treatments and understand the involved mechanisms. Prevent and predict the response to immunotherapies is the key to success.
To discover our associated products and reagents :